India is paying more for less when it comes to Health Insurance: Premium gone up 50-200% for majority over the last 3 years while claims remain very cumbersome
- ● Over 4 in 10 health insurance policy owners surveyed who have made a claim said the insurance company rejected it or only partially approved it for invalid reasons
- ● 5 in 10 health insurance policy owners surveyed who filed a claim said it took between 6 and 48 hours for it to be approved and for them to be discharged from the hospital
March 7, 2026, New Delhi: Recent data from the Insurance Regulatory and Development Authority of India (IRDAI) and industry sources indicate mixed outcomes in health-insurance claim processing and settlement during 2024–26, with several concerns relating particularly to senior citizens.
In FY2024, insurers registered over 3 crore health-insurance claims worth approximately INR 1.2 lakh crore. Of these, around 2.7 crore claims were settled, amounting to INR 83,493 crore. This translates to a settlement rate of about 82% by number, but only 71.3% by value, suggesting that a significant share of claims was either partially settled or rejected.
Claims disallowed amounted to roughly INR 15,100 crore, while INR 10,937 crore worth of claims were repudiated by insurers. The average claim amount stood at about INR 31,086, and nearly 66.16% of claims were processed through the cashless mode, indicating gradual improvements in claim-processing mechanisms.
Despite these improvements, concerns persist regarding settlement practices. Health-insurance complaints increased by 41% to 1,37,361 in FY2025, largely due to claim rejection, delays, and partial settlements. Notably, more than half of the grievances handled by insurance ombudsmen relate to health-insurance claims, highlighting continuing consumer dissatisfaction.
On the flip side, health-insurance premiums have risen over the past two years rather than declining, prompting regulatory scrutiny. In FY2024–25, total health-insurance premiums increased by about 9.19% to INR 1.27 lakh crore, according to IRDAI.
IRDAI has acknowledged that rising premiums are driven primarily by medical inflation and higher claim costs, and has initiated measures to improve predictability, fairness, and transparency in premium revisions. A key regulatory intervention relates to senior-citizen health-insurance policies, where annual premium increases have been capped at 10% unless prior approval is obtained from IRDAI.
In early 2025, IRDAI issued a circular specifying that insurers cannot increase premiums for senior-citizen health-insurance policies by more than 10% in a single policy year without prior regulatory approval. Insurers must also consult IRDAI before withdrawing any senior-specific health-insurance products, ensuring continuity of coverage for older policyholders. This cap addresses long-standing concerns regarding steep and unpredictable premium hikes for seniors, which in some cases had exceeded 30–40%, making coverage increasingly unaffordable. The new framework aims to curb volatility, promote actuarially sound pricing, and prevent abrupt repricing of existing products.
Some insurers have also re-priced older or loss-making product portfolios to maintain viability, which may result in higher-than-average renewal increases in certain cases. Industry commentary attributes recent premium adjustments largely to such commercial and actuarial considerations. For other age groups, there is currently no fixed annual cap on premium increases, although insurers remain subject to actuarial standards and regulatory oversight. Industry observers expect IRDAI to introduce additional consumer-protection measures as medical inflation continues to remain elevated.
IRDAI has reiterated key principles governing premium revisions. Premium increases must be actuarially justified and based on credible claims experience, and insurers must clearly communicate the reasons for any hike at the time of policy renewal. Fresh underwriting cannot be undertaken at renewal solely to penalise policyholders with prior claims, and fundamental policy terms cannot be unilaterally altered during renewal cycles.The regulator has also encouraged insurers to adopt measures to contain underlying healthcare costs, including negotiating standardised treatment package rates with hospitals, which could help moderate future premium increases.
With over a thousand complaints received by LocalCircles on health insurance premium increases and claims just in the last 12 months, the platform conducted a nationwide survey to find out the experience of health insurance policy holders with claims, and how much more they are having to pay when it comes to policy renewal premium. The survey received over 54,000 responses from consumers located in 323 districts of India. 67% respondents were men while 33% respondents were women. 41% of respondents were from tier 1, 32% from tier 2 and 27% respondents were from tier 3, 4, 5 & rural districts.
Over 4 in 10 health insurance policy owners surveyed who have made a claim in the last 3 years said that the insurance company rejected it or only partially approved it for invalid reasons
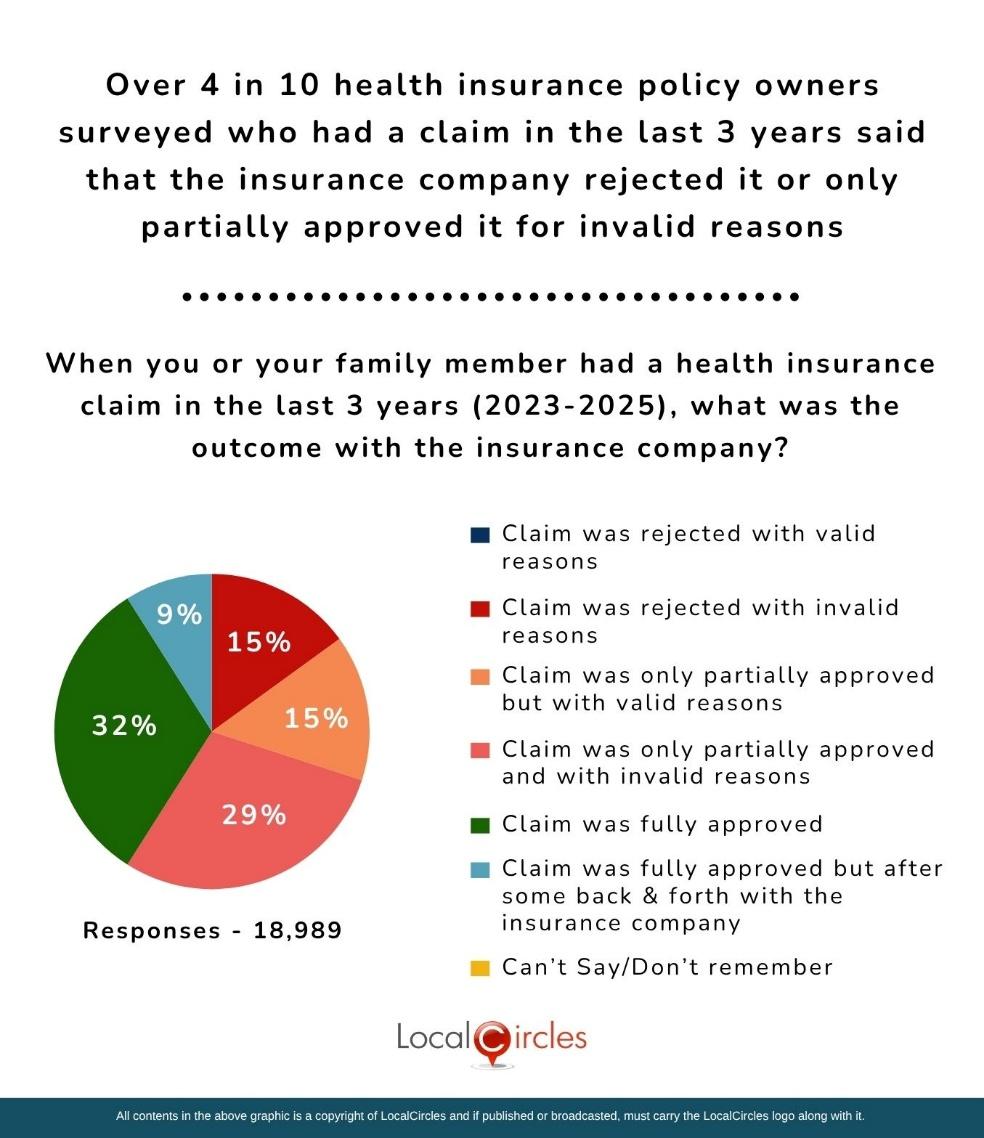
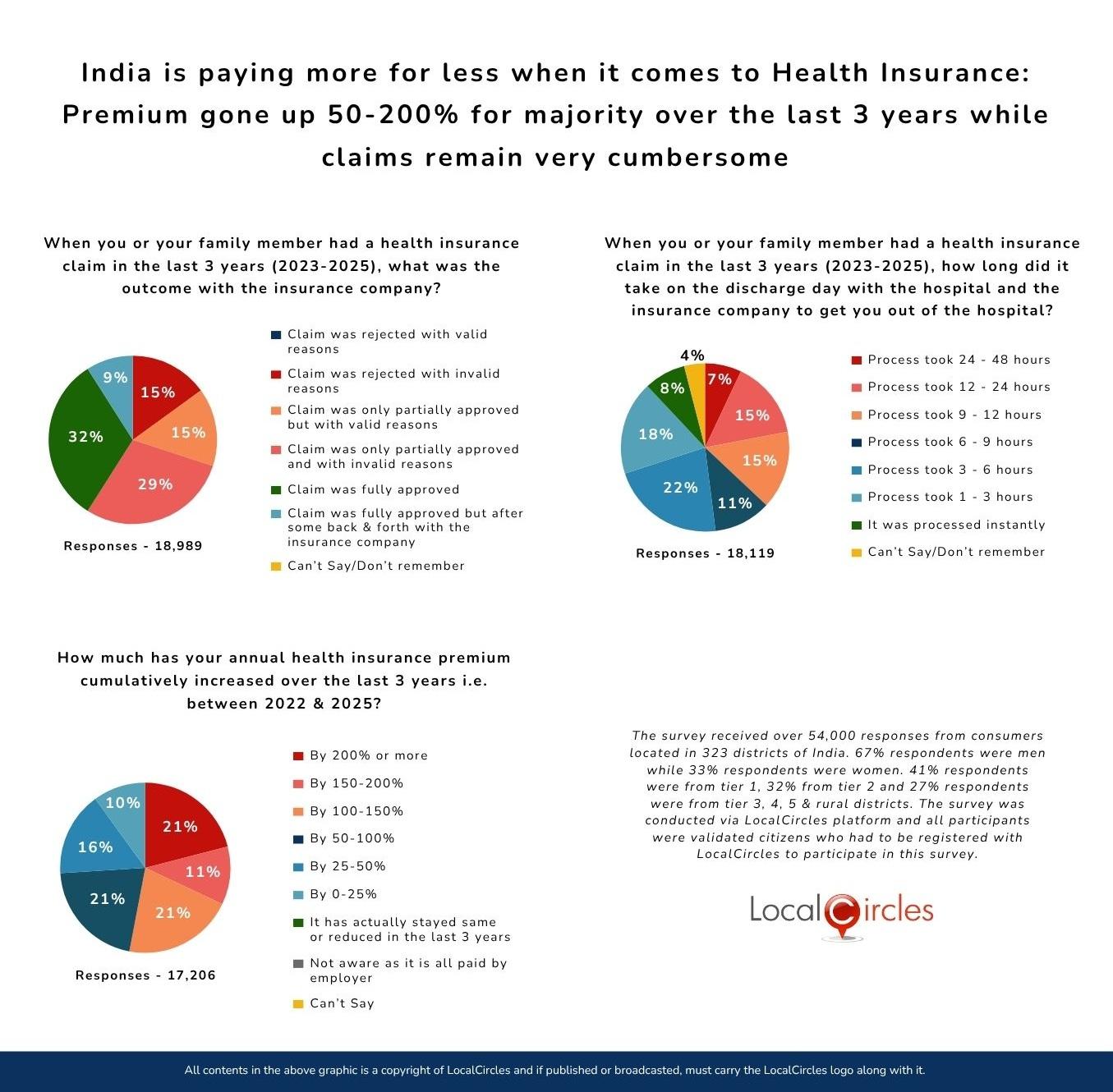
Rejection or delay in settlement of a health insurance claim can be a very harrowing experience which unfortunately many undergo leading to delay in discharge of a patient. It is worse when the patient is no more and the relatives want to get the body for conducting last rites. The survey asked health insurance policy holders, “When you or your family member had a health insurance claim in the last 3 years (2023-2025), what was the outcome with the insurance company?” Out of 18,989 who responded to the question 15% indicated that the “claim was rejected with invalid reasons”; 15% of respondents indicated that the “claim was only partially approved with valid reasons”; 29% of respondents indicated that the “claim was only partially approved with invalid reasons”; 32% of respondents indicated that the “claim was fully approved”; and 9% of respondents indicated that the “claim was fully approved but after some back & forth with the insurance company”. To sum up, over 4 in 10 health insurance policy owners surveyed who have made a claim in the last 3 years said that the insurance company rejected it or only partially approved it for invalid reasons.
5 in 10 health insurance policy owners surveyed who filed a claim in the last 3 years said it took between 6 and 48 hours for their claim to be approved and for them to be discharged
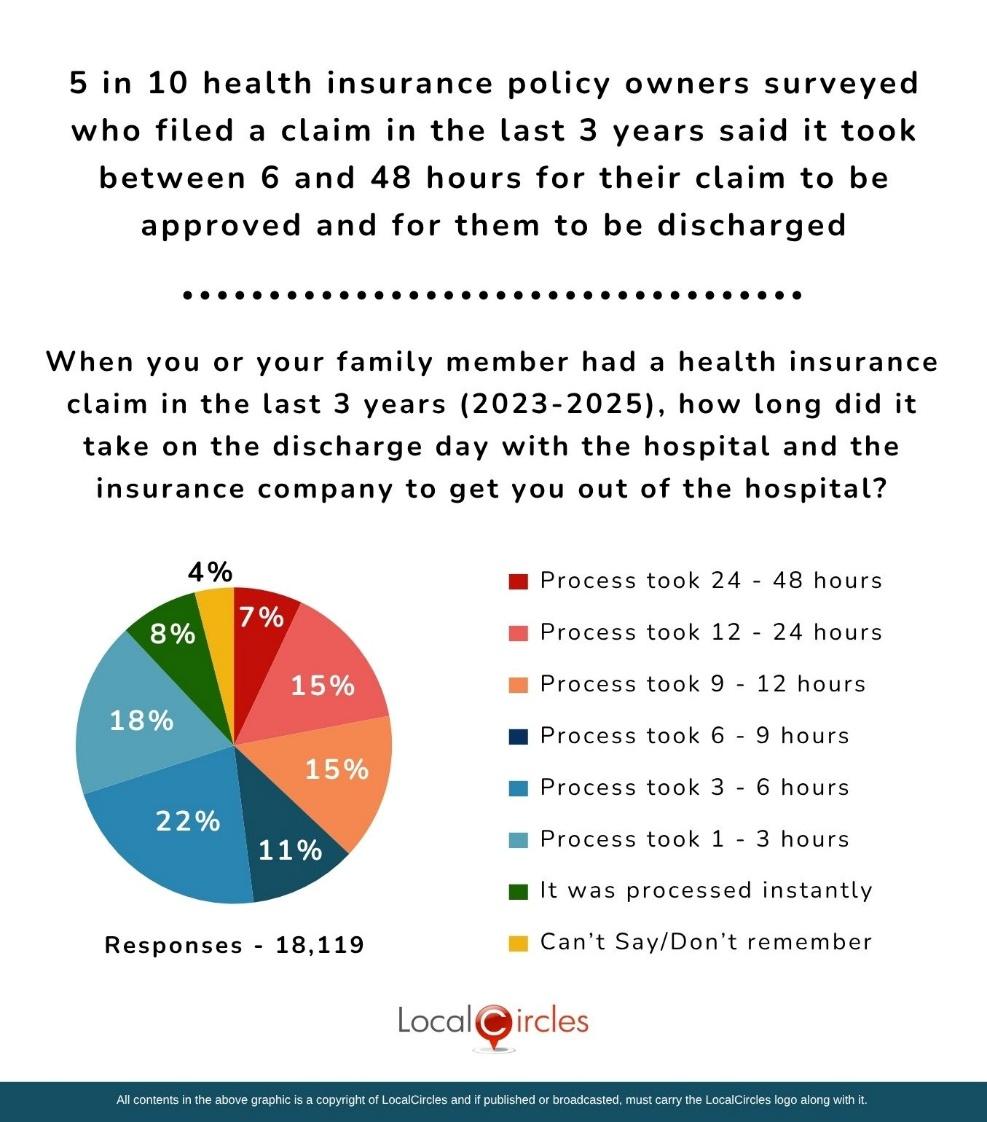
Given that many health insurance policy holders are forced to run around to get their claims reimbursement approved/ settled despite the IRDAI directive that cashless authorization requests should be approved within one hour and finalize discharge authorizations within three hours of receiving the necessary requests from hospitals, the survey asked, “When you or your family member had a health insurance claim in the last 3 years (2023-2025) how long did it take on the discharge day with the hospital and the insurance company to get you out of the hospital?” Out of 18,119 who responded to the question 7% indicated that the “process took 24- 48 hours”; 15% of respondents indicated that the “process took 12-24 hours”; 15% of respondents indicated that the "process took 9-12 hours”; 11% of respondents indicated that the “process took 6-9 hours”; 22% of respondents indicated that the “process took 3-6 hours”; 18% of respondents indicated that the “process took 1- 3 hours”; 8% of respondents indicated that “it was processed instantly” and 4% of respondents did not give a clear answer”. To sum up, 5 in 10 health insurance policy owners surveyed who filed a claim in the last 3 years said it took between 6 and 48 hours for their claim to be approved and for them to be discharged from the hospital.
Over 7 in 10 health insurance policy holders surveyed confirm that their premium increased 50-200% cumulatively over the last 3 years
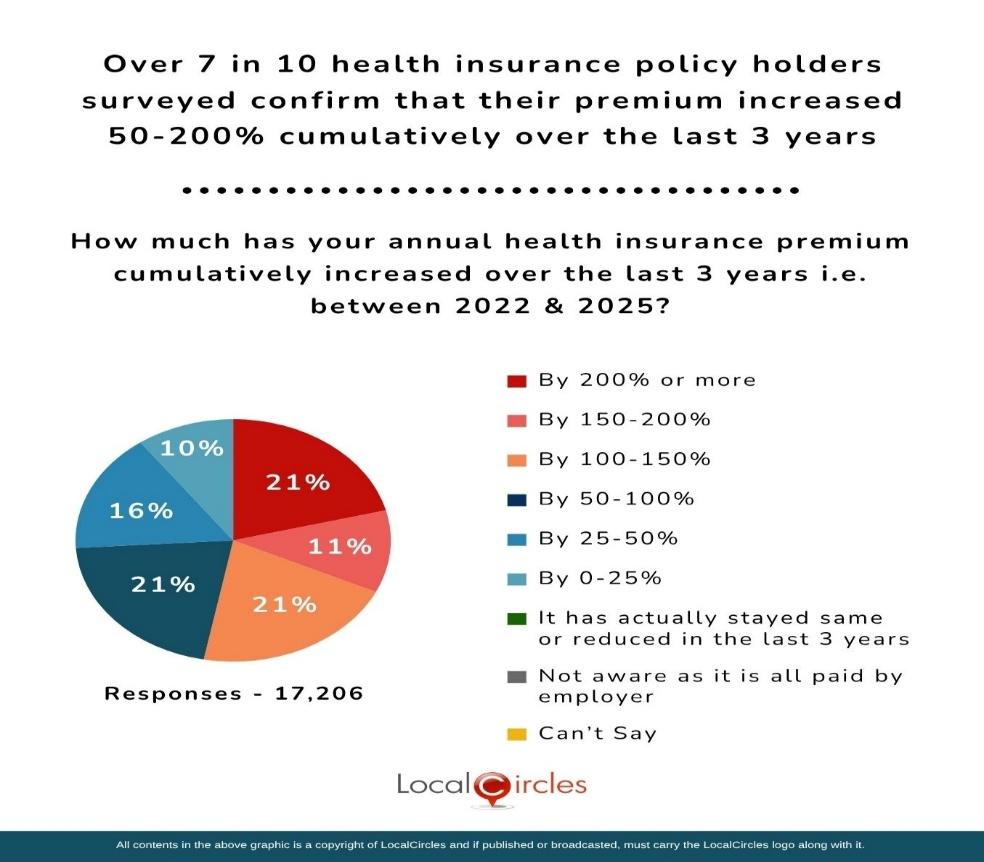
Increase in the annual health insurance policy premium varies from insurance company to company, different packages taken as also the age of the person being insured. The survey asked health insurance policy holders, “How much has your annual health insurance premium cumulatively increased over the last 3 years i.e. between 2022 and 2025?” Out of 17,200 who responded to the question 21% indicated that the increase was “by 200% or more”; 11% of respondents indicated “by 150-200%”; 21% of respondents indicated “by 100-150%”; 21% of respondents indicated "by 50-100%”; 16% of respondents indicated "by 25-50%”; and 10% of respondents indicated "by 0-25%”. To sum up, over 7 in 10 health insurance policy holders surveyed confirm that their premium increased 50-200% cumulatively over the last 3 years.
In summary, the study shows that despite the insurance regulator IRDAI’s directives, over 4 in 10 health insurance policy owners surveyed who have made a claim in the last 3 years said that the insurance company rejected it or only partially approved it for invalid reasons. Similarly, 5 in 10 health insurance policy owners surveyed who filed a claim in the last 3 years said it took between 6 and 48 hours for their claim to be approved and for them to be discharged from the hospital. Despite the IRDAI mandate of cashless health insurance claim processing time of 3 hours, many insurance companies use delaying tactics to buy more time and frustrate policy holders by approving partial claims.
On the premium front, over 7 in 10 health insurance policy holders surveyed confirm that it increased 50-200% cumulatively over the last 3 years which is steep by any standard. While the IRDAI has mandated up to 10% increase for senior citizens, complaints indicate that some companies are still increasing premium above this threshold.
LocalCircles will share this report with the IRDAI and request that process reforms be initiated to ensure timely processing of cashless health insurance claims within the 3-hour mandated window. Similarly on health premium increases, audit or spot check exercises be done to ensure compliance to the 10% premium increase limit for senior citizens.
Survey Demographics
The survey received over 54,000 responses from consumers located in 323 districts of India. 67% respondents were men while 33% respondents were women. 41% of respondents were from tier 1, 32% from tier 2 and 27% respondents were from tier 3, 4, 5 & rural districts. The survey was conducted via LocalCircles platform, and all participants were validated citizens who had to be registered with LocalCircles to participate in this survey.
About LocalCircles
LocalCircles, India’s leading Community Social Media platform enables citizens and small businesses to escalate issues for policy and enforcement interventions and enables Government to make policies that are citizen and small business centric. LocalCircles is also India’s # 1 pollster on issues of governance, public and consumer interest. More about LocalCircles can be found on https://www.localcircles.com
For more queries - media@localcircles.com, +91-8585909866
All content in this report is a copyright of LocalCircles. Any reproduction or redistribution of the graphics or the data therein requires the LocalCircles logo to be carried along with it. In case any violation is observed LocalCircles reserves the right to take legal action.
Enter your email & mobile number and we will send you the instructions.
Note - The email can sometime gets delivered to the spam folder, so the instruction will be send to your mobile as well


